Post-recovery Stigma in Early and Late COVID-19 Epidemic
Article information
Abstract
People who recover from the novel coronavirus diseases 2019 (COVID-19) complain of psychological symptoms such as stress, anxiety, and depression by psycho-stress due to social stigma in the early stage of the epidemic. To assess the psychological stigma of early and late epidemic periods, stigma scale was compared between the first epidemic period (February-May 2020, n = 20) and the fifth epidemic period (February-May 2022, n = 21) post-recovery COVID-19 patients in outpatient clinic. The average total stigma score was significantly higher (79.6 ± 18.16) in post-recovery COVID-19 patients of the early (first) epidemic period compared to late (5th) epidemic period patients (37.5 ± 10.99). Four subscales were significantly higher in early epidemic period compared to late epidemic period (enacted stigma 27.5 ± 7.25 vs. 13.0 ± 4.18, disclosure concerns 19.5 ± 9.38 vs. 9.4 ± 2.99, negative self-image 16.2 ± 8.10 vs. 8.1 ± 2.47, concern with public attitudes 16.6 ± 6.95 vs. 7.0 ± 2.01). In those who recovered from the early COVID-19 epidemic period, patients experienced significantly higher social stigma stress compared to the late epidemic period. In the early period of novel virus epidemics, the risk of personal stigmatization and stress should be prevented in public policy. Socio-psychological assessment and treatment should be considered for the patient in addition to physical symptoms.
Introduction
The novel coronavirus diseases 2019 (COVID-19) epidemic is a unique and rare global disaster situation for the current generation, and even those who have recovered from the infection are complaining of physical symptoms such as fatigue and helplessness, and psychological symptoms such as stress, anxiety, and depression [1].
The Affected population can experience a variety of psychological stress and stigma due to the fear of spreading the disease to others. In the first epidemic period (February-May 2020), COVID-19 patients from some religious groups are faced public criticism and stigmatization that they violated quarantine policy and caused mass outbreaks. Social activity and movement of citizens were restricted by quarantine policy. Affected patients suffered from the burdens of the disease and from the stigma of being the host for transmitting the disease among community members [2].
Diseases caused by infection-related stress during the epidemic include ‘COVID stress syndrome’ and ‘long COVID or post-COVID conditions’. ‘COVID stress syndrome’ is a dysfunctional syndrome that includes fear of SARS-CoV2 infection, fear of economic impact, fear of foreigners, compulsive checks and checks, and traumatic stress symptoms associated with infection [3]. ‘Long-term COVID syndrome’ is symptoms that persist for weeks to months after treatment of infection [4].
The aim of the study is to compare the stigma scale of people who recovered from COVID-19 in the early epidemic period (February-May 2020) and the late epidemic period (February-May 2022).
Materials and methods
To assess the psychological stigma of patients admitted and discharged during the early COVID-19 pandemic, it was approved by the Institutional Ethics Review Board (approval number: 2020-03-114). In order to assess the psychological stigma of patients, 20 patients who were discharged after inpatient treatment at one COVID-19 specialized hospital during February-May 2020 evaluated the stigma scale after explaining the purpose of the study. The same questionnaire was evaluated in the late epidemic period (February-May 2022) in the same hospital. In order to collect basic information of study participants, data were collected on a total of six items: gender, age, severity of symptoms (asymptomatic, mild, pneumonia), length of stay in a hospital or residential treatment center, and date after discharge.
The Janice’s stigma scale of AIDS patients [5] was modified to match COVID-19. This test method consists of a total of 32 items and is evaluated on a scale of 128 points. Subdomain factors are assessed in four areas: enacted stigma, disclosure concerns, negative self-image, and concern with public attitudes. Each item was marked on a Likert 4-point scale as very no (1 point), no (2 points), yes (3 points), and very yes (4 points).
Statistical analysis was used by IBM SPSS Statistics ver. 23.0 (IBM Co., Armonk, NY, USA), P values are calculated by Mann-Whitney U test.
Results
Demographic and sociological characteristics
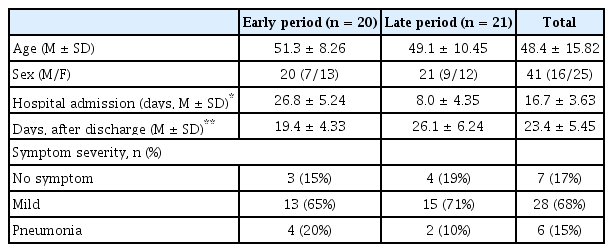
The mean age of the subjects was 50 years old, and the male/female ratio was 16/25 (early 7/13, late 9/12), with 61% women. The average length of stay in hospital and in residential care centers was 27/8 (early/late) days, and the difference in length of stay between the two groups was due to differences in COVID-19 management guidelines (early-isolated admission 14-60 days, late-residential treatment centers 7 days) in the early and late period. The severity of symptoms was 7 (17%) asymptomatic, 28 (68%) mild, and 6 (15%) pneumonia (severe), with no difference between the early (15%, 3/20) and late (19%, 4/21) period (Table 1).
Stigma scale
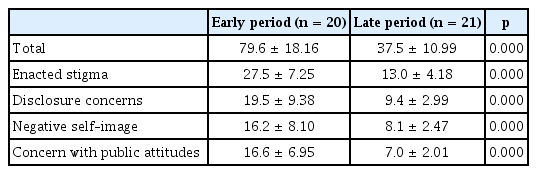
The average total stigma score was significantly higher in early period COVID-19 patients 79.6 ± 18.16) compared to late period patients 37.5 ± 10.99). The mean scores for the four subscales were 20.5 ± 4.21 for enacted stigma, 20.2 ± 3.82 for disclosure concerns, 17.9 ± 3.53 for negative self-image, and 20.9 ± 4.38 for concern with public attitudes. There were significantly higher subscales in the early period of epidemics patients compared to late period patients (enacted stigma 27.5 ± 7.25 vs. 13.0 ± 4.18, disclosure concerns 19.5 ± 9.38 vs. 9.4 ± 2.99, negative self-image 16.2 ± 8.10 vs. 8.1 ± 2.47, concern with public attitudes 16.6 ± 6.95 vs. 7.0 ± 2.01) (Table 2).
Discussion
In comparing stigma scale between the early period of the COVID-19 epidemic (the first epidemic wave) and the late period (the fifth epidemic wave, 2 years later), there were significant differences in stigma stresses in people who recovered after treatment.
Stigma can be defined as a process by which individuals with devalued physical, behavioral, or medical attributes experience prejudice, discrimination, and stereotyping [6]. Stigmatization can delay the diagnostic testing process and increase the epidemics [7]. Because perceptions of stigma can impact the well-being of affected people, it is important to be able to measure the stigma perception of these individuals, especially in the early period.
There are four subscales in Janice’s stigma scale: personalized stigma, disclosure concerns, negative self-image, and concern with public attitudes. The ‘personalized stigma’ subscale deals with the outcomes of others knowing about the individual's status as infected and is related to personal experience of rejection. ‘Disclosure concerns’ are related to the perceived need to control information and keep one's infection status concealed. Items on the ‘negative self-image’ subscale deal with feelings of being not as good as others, and items expressing guilt or shame. The final subscale, ‘concern with public attitudes’, measures what the person with HIV/AIDS believes other people might think about him or her [8].
At the beginning of the epidemic, it can be thought that the unknown course of the disease, the fear of infecting others, and the public criticism of the infected person caused stress to the patient even after the diagnosis of cure. Forty percent of early patients were aware of severe stress, compared to 14 percent of later patients, who were aware of their experience of COVID-19 infection as severe stress even after treatment. In the early stages of the epidemic, COVID-19 infection itself acts as an acute trauma, so it will be necessary to suspect acute stress disorder.
Unlike normal fear, which is a response to an actual threat, we may feel anxious about COVID-19, an unknown and unknown threat. Anxiety appears when we believe and anticipate the possibility of a dangerous or unfortunate event, and can manifest as a variety of physical and psychological symptoms in stressful situations, including feelings of helplessness, despondency, and sadness [9]. At the beginning of the pandemic, anxiety and depression about the unknown disease of COVID-19 infection were severe, but after 2 years of epidemic waves, anxiety can decrease due to public infection control and the availability of vaccines and treatments.
People infected with COVID-19 may feel threatened by public obligatory quarantine and be traumatized mentally [9]. Even after recovery, psychosomatic symptoms can superimpose to the ‘COVID stress syndrome’ and ‘long COVID conditions’. During the initial acute stress period of the epidemic, the phenomenon of stigmatizing and blaming the infected person was shown, and after recovering from the infection, the person experienced considerable stress, anxiety, and depression.
The pandemic experienced for the first time in 2020 in Korea is causing a lot of human and economic damage, but the scale of the epidemic is gradually decreasing as it passes through the several waves for 2-3 years. In the acute early stages of the epidemic, there was a lot of psychological stress for patients due to the fear about unknown diseases. And as the development of COVID-19 vaccines and the effective therapeutics were produced, social anxiety and the psychological burden experienced by individuals decreased.
The limitations of this study were: first, we were unable to investigate a large number of patients due to patient reluctance to complete the questionnaire by psycho-social stress. Secondly, we were unable to investigate patient cases by disease severity or treatment institution (hospital, residential treatment center, home care) due to limitation of the case numbers.
In those who recovered from treatment at the beginning of the COVID-19 epidemic, we found that they experience significant social stigma stress during the first wave and decreased stigma in the later period of the epidemic. During a novel epidemic, both socio-psychological problems and physical symptoms should be assessed and managed considering the sigma stresses. Further long-term research on COVID-19 related stress syndrome and long COVID syndrome is need to be done to prepare to another future epidemics.
Notes
Conflict of interest
The authors declare no conflicts-of-interest related to this article.