Introduction
Eisenmenger syndrome is characterized by hypoxia and pulmonary arterial hypertension due to increased pulmonary vascular resistance (PVR) by intracardiac shunt of blood flow connection between the systemic and pulmonary circulation [1]. The life expectancy of patients with Eisenmenger syndrome is 30-40 years, with rare cases surviving up to 50-70 years. The longer these patients survive, the more likely they are to undergo non-cardiac surgery [2]. When patients with Eisenmenger syndrome undergo non-cardiac surgery, the mortality rate is 20–30% [3], which increases the risk of surgery and requires considerable caution in anesthetic management. In particular, when performing general anesthesia in Eisenmenger syndrome, cardiopulmonary collapse due to risk factors such as a decrease in systemic vascular resistance (SVR), exacerbation of pulmonary hypertension during or after ventilator weaning, and postoperative pain are the most serious concerns for anesthesiologists. A few cases have reported that regional anesthesia, such as cervical plexus block [4], and sciatic and femoral nerve block [5], was safely performed in non-cardiac surgery for patients with Eisenmenger syndrome to minimize complications related to general anesthesia. In this case, we report the successful anesthetic management and pain control by performing ultrasound guided supraclavicular brachial plexus block (BPB) for open reduction with internal fixation of a humerus fracture in a patient with Eisenmenger syndrome.
Case
A 68-year-old woman, 158 cm in height and 47 kg in weight, presented to the orthopedic department of our hospital with a right humerus fracture following slipping. She was diagnosed with Eisenmenger syndrome 3 years earlier and was irregularly taking spironolactone (25 mg qd), furosemide (20 mg qd), and sildenafil (20 mg tid). The patient was recommended for surgery for atrial septal defect (ASD) and right ventricular failure 13 years earlier, but repair was not performed because of the patient’s refusal. She usually complained of exertional dyspnea (New York Heart Association Class II-III). At the time of hospitalization, the patient had a blood pressure (BP) of 106/65 mmHg, heart rate (HR) of 90 bpm, a breathing rate of 20 breaths/min, and body temperature of 37.6℃. A pansystolic murmur in the 4th intercostal space and a loud P2 were also auscultated. Preoperative electrocardiogram (ECG) showed right bundle branch block (RBBB) with anterolateral T wave inversion. Posteroanterior chest radiography showed cardiomegaly and left and right atrial enlargement with pulmonary vasodilation. Transthoracic echocardiography revealed a bidirectional shunt through a large secondum ASD (deficiency size: 4.57 cm), severe pulmonary hypertension (mean pulmonary artery pressure of 46.4 mmHg by measurement of maximum velocity in pulmonary regurgitation), left and right atrium enlargement, right ventricle (RV) hypertrophy, and moderate tricuspid regurgitation. There was no regional wall motion abnormality in the left ventricle (LV) wall, and the ejection fraction was 65%. Her pulmonary function test recorded moderate obstructive ventilatory defect with a forced expiratory volume in one second (FEV1) of 0.83 L (46%), and a FEV1/forced vital capacity ratio of 68%. The laboratory findings were within the normal range. Based on the patient’s history and preoperative tests, it was concluded that the patient belonged to a high-risk group under general anesthesia after consultation with the cardiology and respiratory medicine department. Therefore, open reduction with internal fixation in the right humerus was planned under supraclavicular BPB.
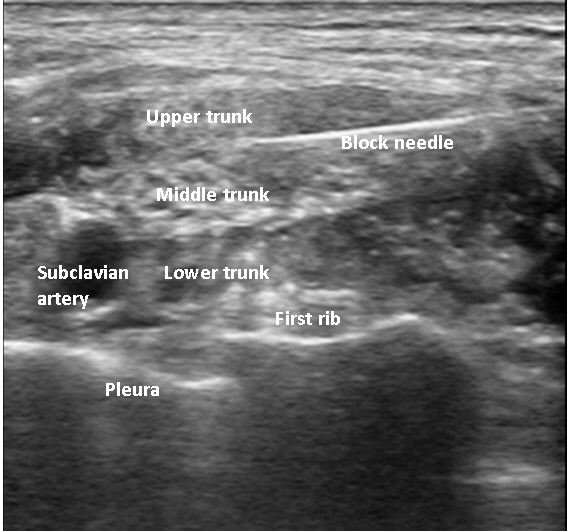
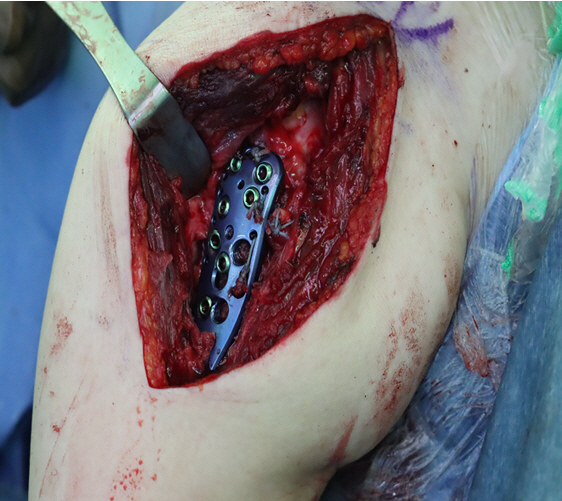
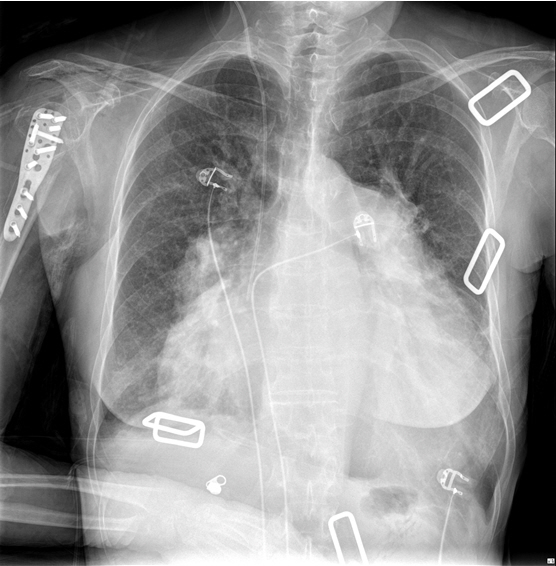
Upon the patient’s arrival in the operating room, the pre-anesthesia vital signs were as follows: non-invasive BP, 147/89 mmHg; RBBB on ECG with HR of 80 bpm, 93.4% peripheral oxygen saturation (SpO2). The patient complained of dyspnea in the supine position. Therefore, left radial arterial catheterization and ultrasound-guided central venous catheterization in the right internal jugular vein were performed while maintaining the position of the patient’s upper body lifted approximately 30 degrees with O2 at 3 L/min. After turning the patient’s head in the opposite direction to the procedure, the neck and chest areas around the right clavicle were sterilized with iodine solution, and a sterile fenestrated drape was covered. A 5- to 13-MHz linear probe (UST-5411, Hitachi Aloka Medical, Tokyo, Japan) of ultrasound was placed on the clavicular fossa and scanned to visualize the brachial plexus appearing as a bundle of hypoechoic circular nodules, which was located lateral to the pulsating subclavian artery lying on the first rib. A 50-mm 22-G insulated needle (Stimuplex® Insulated; B. Braun, Melsungen, Germany) was inserted laterally to medially into the brachial plexus sheath using the in-plane technique. The trajectory of the needle was adjusted to place 0.75% ropivacaine around the lower, middle, and upper trunks (Fig. 1). A total of 187.5 mg of 0.75% ropivacaine (25 mL) was used to perform a supraclavicular brachial plexus block. Twenty minutes after placement of the BPB, sensory blockade of the C5-to-T1 dermatome and the surgical site was evaluated by applying an alcohol-soaked sponge to the skin areas corresponding to each dermatome [6]. Anesthesia was determined to be appropriate for surgery in the absence of cold sensations at the surgical site. However, the loss of cold sensation in all dermatomes was not mandatory to determine the appropriate anesthesia for surgery. Motor blockade was not assessed because movement of the upper limb could aggravate injury related to the fracture. The patient’s position was changed to a 70- to 80-degree sitting position before surgery began. After position change, arterial BP was 136/64 mmHg, HR was 97 bpm, SpO2 was 99%, and central venous pressure (CVP) was 3.8 mmHg. She complained of severe anxiety and dexmedetomidine was continuously infused at a rate of 0.5 µg/kg/h without loading dose to induce and maintain natural sleep during the surgery. Forty minutes after the surgery began, the systolic and diastolic arterial BP gradually decreased to 90/49 mmHg, necessitating continuous infusion of norepinephrine at a rate of 0.05−0.1 µg/kg/min. Throughout the surgery, the BP and HR were maintained at 90−110/45−58 mmHg and 65−70 bpm, respectively. Arterial blood gas analysis performed 10 min before the end of the operation showed a pH of 7.406, PaCO2 of 44.7 mmHg, PaO2 of 130 mmHg, and base excess of 2.8 mmol/L. The operation was completed without any events or additional administration of analgesics or sedative agents during surgery (Fig. 2). There was no pleural effusion or elevation of right hemidiaphragm due to phrenic nerve palsy in postoperative chest radiography (Fig 3). The duration of anesthesia and surgery was 171 and 93 min, respectively. The amount of fluid intravenously administered during the operation was 598 mL, and the estimated intraoperative bleeding volume was 300 mL.
After surgery, the patient was transferred to the post-anesthesia care unit while administering oxygen at 3 L/min via a nasal cannula. Norepinephrine infusion was continued, which maintained arterial BP and HR at 123−107/67−59 mmHg and 70−73 bpm, respectively. The norepinephrine infusion rate was tapered, and the infusion was finally stopped 30 min after the surgery, when BP and HR were maintained at 108−103/58−57 mmHg and 63−73 bpm, respectively, without any interval change in the ECG. The patient did not complain of postoperative pain and did not present cardiopulmonary symptoms. The patient returned to the ward where oxygen was administered at a rate of 3 L/min at 48 h after surgery. SpO2 was maintained at 87−96% without oxygen supply. The patient was discharged on the 9th postoperative day without any complications.
Discussion
Eisenmenger syndrome is a pulmonary vascular disease in which a large amount of blood flows into the pulmonary artery due to congenital heart diseases such as uncorrected ventricular septal defect, ASD, or patent ductus arteriosus, subsequently thickening or obstructing the wall of the pulmonary artery [7]. In these patients, a left-to-right shunt due to ASD increases blood flow to the pulmonary artery and PVR, resulting in pulmonary hypertension. Over several decades, hypertrophy of the right atrium and RV with shunt reversal eventually leads to right-sided heart failure and bidirectional shunts. This results in a systemic hypoxic state with symptoms, such as cyanosis and exertional dyspnea [7, 8].
Anesthetic management of patients with Eisenmenger syndrome is challenging for anesthesiologists. It is particularly important to maintain an appropriate level of SVR and PVR. At the time of induction under general anesthesia, PVR decreases when using propofol but not when using thiopental [9]. However, blood pressure significantly drops as SVR decreases, and the use of a vasopressor might be necessary [3]. A sharp decrease in SVR leads to impairment of diastolic filling due to pushing of the RV toward the LV cavity, decreased cardiac output, and myocardial ischemia [10]. Ketamine increase SVR through sympathetic activation and also increase PVR. Etomidate has little effect on PVR and RV contractility, enabling safe usage in patients with pulmonary hypertension [9]. Inhalational anesthetic agents decrease RV function by reducing contractility, preload, and afterload [11]. In particular, desflurane and nitrous oxide increase PVR [12, 13]. In addition, general anesthesia-related situations such as stimulation by an endotracheal intubation device such as a laryngoscope, high airway pressure and partial pressure of end-tidal CO2, and positive pressure mechanical ventilation during anesthesia are factors that increase PVR [14]. Increased intrathoracic pressure and tachycardia during ventilator weaning also caused an increase in PVR. Therefore, our patient with Eisenmenger syndrome was at a high risk for general anesthesia.
If upper extremity surgery is required in patients with Eisenmenger syndrome, BPB could be an alternative to general anesthesia. Supraclavicular BPB involves the trunks and division level of the brachial plexus and is suitable for arm surgery. It is known that half of patients with supraclavicular BPB experience phrenic nerve palsy [15] but usually no symptoms at rest. In addition, other complications such as pneumothorax may occur. However, the incidence of abovementioned complications could be reduced by ultrasound guided technique. It has been reported that ultrasound guided supraclavicular BPB with 20 mL of 0.75% ropivacaine significantly reduced hemidiaphragmatic paresis compared to the use of a nerve stimulator [16]. In our case, the patient had exertional dyspnea and moderate obstructive pattern in pulmonary function test, but ultrasound guided supraclavicular block was performed successfully without pulmonary complication. This suggests that supraclavicular BPB can be performed safely through ultrasound guidance, even in patients with poor pulmonary function.
Other cases of performing supraclavicular BPB in patients with pulmonary hypertension have been published. Sakuta et al. [17] reported that hemidiaphragmatic paresis and need for ventilator support occurred after supraclavicular BPB with 30 ml of 0.75% ropivacaine under ultrasound guidance for revision of arteriovenous fistula on the arm in moderate pulmonary patients with chronic renal failure, prosthetic mitral valve, and pacemaker. After one week, the re-operation was performed without complications under the supraclavicular BPB using 20 ml 0.75% ropivacaine. Afonso and Beilin [18] also reported respiratory failure after administration of 40 ml of 1.5% mepivacaine and 15 ml of 1% lidocaine under ultrasound guidance for arteriovenous graft insertion in a patient with pulmonary hypertension accompanied by chronic renal failure, asthma, and obesity (BMI > 40 kg/m2). They suggested that the amount of local anesthetic in BPB should be adjusted or reduced considering the presence of other underlying diseases, such as chronic renal failure and cardiopulmonary disease, in addition to pulmonary hypertension. It is important to use ultrasonography not only to prevent overuse of local anesthetic, but also to administer an appropriate dose for sufficient block as a surgical anesthesia. Further studies on the optimal amount of local anesthetic when performing BPB in patients with pulmonary hypertension are needed.
When performing BPB, sympathetic nervous system activity decreases, and vasodilation results in decreased SVR and increased blood flow in the upper extremity. However, these effects of BPB are localized to the arm and shoulder compared to those of general anesthesia. In addition, because elevation of sympathetic tone due to inadequate analgesia could increase PVR [19], BPB is safe and beneficial to patients in terms of postoperative pain control. Therefore, we performed supraclavicular BPB to minimize the systemic effects of anesthesia and for upper arm surgery through deltopectoral approach. Although BPB has less systemic effects than general anesthesia, hypotension occurred during surgery in our patient as well. Several factors, such as dexmedetomidine, BPB, sitting position, and intraoperative bleeding, are thought to cause hypotension. A decrease in SVR in patients with Eisenmenger syndrome worsens shunt and RV failure. This leads to LV diastolic dysfunction and decreased cardiac output. Therefore, intraoperative hemodynamic changes in Eisenmenger syndrome require closer monitoring for continuous blood pressure fluctuations through arterial catheterization before induction and prompt treatment [3]. It is also important to use vasopressors to prevent a decrease in SVR and ultimately increase coronary blood flow [11]. In our case, norepinephrine was used; it is known to increase systolic BP over a wide range and reduce pulmonary arterial pressure less than phenylephrine in patients with chronic pulmonary hypertension [20]. Strict fluid administration during surgery is also important in patients with pulmonary hypertension because they are in a hypovolemic state with long-term diuretic use. In our case, we controlled the rate of fluid administration based on preoperative CVP, intraoperative blood loss, and maintenance fluid dose per body weight to prevent hypervolemia.
Considering the patient’s anxiety before surgery, we decided to administer a dexmedetomidine infusion for intraoperative sedation. Dexmedetomidine is an alpha-2 agonist with sedative and analgesic effects and causes less respiratory depression than other sedative agents. Therefore, perioperative factors that increase PVR, such as hypoxia, hypercarbia, acidosis, and pain, can be reduced [21]. Ebert et al. [22] reported that administration of dexmedetomidine at a low concentration (< 1.9 ng/mL) did not increase mean arterial pressure, SVR, or PVR but increased it at a high concentration. It is assumed that the vasoconstrictive effect of alpha-2B receptor activation is predominant when dexmedetomidine is administered at a high concentration. Studies on the safety of perioperative dexmedetomidine in patients with pulmonary hypertension are rare. One case reported that 0.2−0.4 µg/kg/h dexmedetomidine was used safely as monitored anesthetic care without complications in patients undergoing inguinal hernioplasty under peripheral nerve block [23]. It has also been reported that the use of dexmedetomidine (0.5 µg/kg/h) for sedation and analgesia in patients with severe pulmonary hypertension, pneumonia, and cardiopulmonary failure can not only control pain but also avoid tracheal intubation and positive pressure ventilation [21]. Therefore, the use of dexmedetomidine in patients with Eisenmenger syndrome, especially low-concentration infusion, is safe in terms of having anxiolytic and analgesic effects as well as maintaining hemodynamic stability for sedation.
In conclusion, supraclavicular BPB for upper extremity surgery in a patient with Eisenmenger syndrome is considered a safe anesthetic technique in terms of not only fewer hemodynamic changes such as decreased SVR and increased PVR compared to general anesthesia, but also ease of postoperative pain control.